Achilles tendinopathy is a common problem many athletes experience. While there are a wide variety of treatments utilized in the rehab world that claim to have benefits, successful, long-term outcomes are usually dependent upon one variable. Load management!
Achilles Tendinopathy
Despite being one of the largest tendons in the body, the Achilles tendon is one of the most frequently injured, especially in those participating in running and jumping activities.
Characterized by a combination of pain, swelling, and decreased athletic performance, Achilles tendinopathy is commonly associated with training errors such as rapidly increasing training intensity or duration.
While your physical therapist may jump to common treatments such as stretching, cross-friction massage, iontophoresis, or electric stimulation, the most important part of the rehabilitation process should ALWAYS be on how to properly LOAD the tendon!
Classifying Tendinopathy
Recent research by Cook and Rio shed light on how to accurately classify tendinopathy. While the pathogenesis is more in-depth, generally speaking, tendinopathy can be classified into either a “reactive” or “degenerative” category.
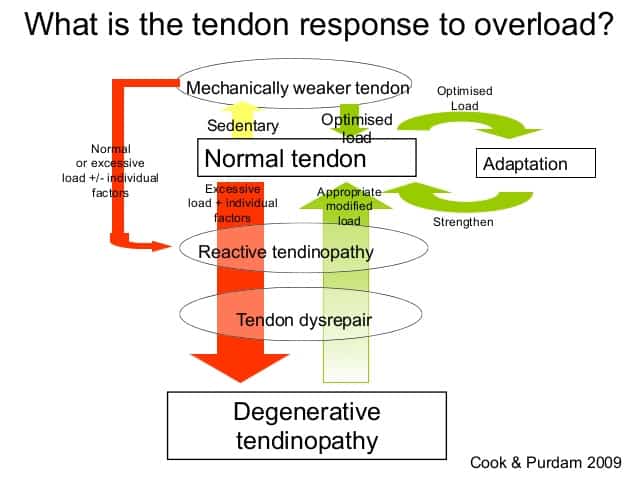
A pathology model to explain the clinical presentation of load-induced tendinopathy (Cook and Purdam 2009)
While degenerative Achilles tendinopathy, a chronic condition usually seen in the older population, is certainly an area of concern, this article will outline load management strategies for reactive tendinopathy, as it is more common in the every day athlete.
Reactive Tendinopathy
Reactive Tendinopathy is characterized by acute pain. This is usually due to a doing “too much, too fast, too soon” a.k.a an acute overload event that the trainee was unaccustomed to.
Traditionally, this issue was looked at as an inflammatory condition and treated with various techniques such as soft tissue mobilization, stretching, iontophoresis, electrical simulation, and/or ice. Recently, however, we’ve come to realize, there may be a more optimal way to treat this!
Calm Down Reactive Tendinopathy with Isometrics
While passive modalities have typically been used to treat acute “tendinitis” (now reactive tendinopathy), research shows us that isometrics also have a similar analgesic effect. Additionally, they are something that patients can perform by themselves, promoting an internal locus of control and self efficacy.
For reactive Achilles tendinopathy, start with isometric bilateral heel raises for 3-4 sets of 20-45 seconds each, multiple times a day. Pain shouldn’t be more than a 3 out of 10 during, should feel slightly better immediately upon stopping, and should also not be worse the following day. This is evidence of a successful treatment.
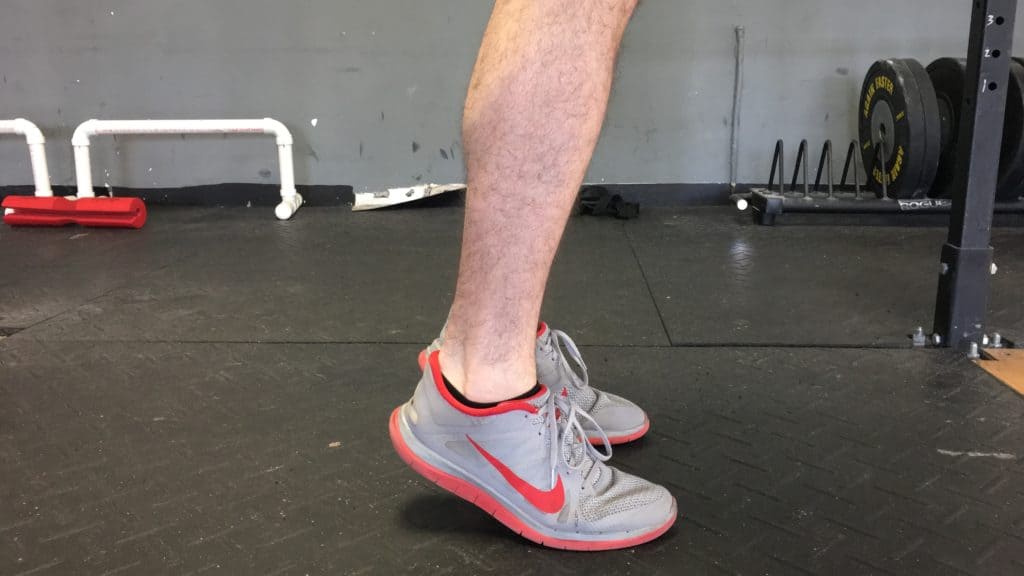
Demonstration of isometric heel raise. Hold this position for 20-45 sec. Don’t judge my lack of calf hypertrophy!
While eccentric heel raises have their place in treating Achilles tendinopathy, if prescribed too early (specifically in the reactive phase) it can actually increase pain. Stick with the isometrics early on!
What About Other Modalities?
Here’s the truth. While manual therapy, modalities, or cross-friction massage CAN be a part of successfully managing Achilles tendinopathy, they aren’t absolutely necessary for pain reduction and positive outcomes. Studies show positive outcomes with load management alone!
If you utilize manual therapy for tendinopathy as a way to modulate pain and promote buy in to your therapeutic exercise, I can see that. Just know you’re probably not breaking down any “adhesions” or remodeling the tendon with your hands! I’ve said it before and will say it again…your body is more resilient than that!
Build Tendon Strength with Heavy Resistance Training
Once pain has subsided with properly dosed isometrics, it’s time to build up that tendon strength! Historically, we’ve relied on eccentric exercise to achieve this, but recent evidence shows similar outcomes with also incorporating the concentric portion.
To perform this heavy resistance training, utilize a 3-second concentric phase and a 3-second eccentric phase for a 6-second rep of a heavy load. Exercises such as the standing and seated barbell calf raises work perfect for this.
Standing barbell calf raises performed with a 3-second concentric, and 3-second eccentric.
Seated barbell calf raises performed with a 3-second concentric, and 3-second eccentric.
Stable vs. Irritable Response
Regarding dosage, start with or 3-4 sets of 15 reps and progress to lower reps (6-8). Again, some pain is allowed, up to 3/10, but it should subside by the next day! Usually, tendons don’t like to let you know you’ve done too much until the day after the activity. So training doesn’t need to be “pain-free” but it should be tolerable!
If you experience a flare-up 24 hours after the exercises, I’d recommend manipulating some training variables such as decreasing the intensity or volume.
Once tendon strength is improved, the athlete can then resume regular training sessions and eventually return to sport.
It should be noted that while this article solely focuses on techniques to load the Achilles, it is also important to concurrently take a global approach and address other areas such as balance, proprioception, and general lower body strength!
Conclusion
Gone are the days of relying on iontophoresis, cross-friction massage, and electrical stimulation to treat Achilles tendinopathy. Successful outcomes are dependent upon the simple principle of load management.
Use isometrics to calm down reactive Achilles tendinopathy, and build strength with heavy loaded resistance training!

